Is It Good Tgat Gestational Sac Measuring Same as My Charting but No Baby 6.4
1st Trimester Ultrasound Scanning
Technique · Gestational Sac · Yolk Sac · Fetal Middle Trounce · Fetal Pole · Crown Rump Length · Gestational Age · Twins · Missed Ballgame · Threatened Abortion · Incomplete Abortion · Ectopic Pregnancy · Corpus Luteum Cyst · Nuchal Translucency Thickness
First trimester scanning is useful to identify abnormalities in the early evolution of a pregnancy, including miscarriage and ectopic pregnancy, and provides the most accurate dating of a pregnancy.
Technique
First trimester scanning can be performed using either an intestinal approach or a vaginal approach. Abdominal scanning is performed with a full maternal bladder, provides a wider field of view, and provides the greatest depth of view. Vaginal scanning is best performed with the bladder empty, gives a much greater resolution with greater crispness of fine detail. In circumstances where both approaches are readily bachelor, the greater particular provided past transvaginal scans usually outweighs other considerations, and is preferred.
The patient is scanned in the normal examination position (dorsal lithotomy) with her feet secure in stirrups and her perineum even with the terminate of the test table. Place a small-scale corporeality of ultrasonic coupling gel on the tip of the transvaginal transducer. And then embrace the transducer with a rubber. After lubricating the vaginal opening, gently insert the transducer into the vagina.
Visualize the longitudinal plane of the uterus (sagital department) and evaluate its' size. It can be measured from the cervix to the fundus, AP diameter, and width. Normal uterine volume is less than 100 cc (nulliparous patients) and less than 125 cc (multiparous patients). Identify (if present), the gestational sac, yolk sac, fetus (or fetuses), presence or absence of fetal movement and fetal heart beat.
After the uterus is evaluated past sweeping upward and down and side to side, the ovaries are identified and evaluated. This is most easily achieved by first identifying the internal iliac vessels. The ovaries are ordinarily located merely anterior to the iliac vessels.
Document important views and measurements on moving-picture show or electronically. Then document your findings in some written format.
1st Trimester Ultrasound Scan
Gestational Sac
The gestational sac is the earliest sonographic finding in pregnancy. The gestational sac appears as an echogenic (brilliant echoes) ring surrounding a sonolucent (clear) center. The gestational sac does not correspond to specific anatomic structures, but is an ultrasonic finding characteristic of early pregnancy. Ectopic pregnancies can as well have a gestational sac identified with ultrasound, even though the pregnancy is not inside the endometrial cavity.
The gestational sac first appears at virtually 4 weeks gestational age, and grows at a rate of almost ane mm a day through the 9th week of pregnancy.
Your ability to identify an early gestational sac will depend on many factors, including the capabilities of the ultrasound equipment, your arroyo (vaginal or abdominal), your experience, the orientation of the uterus (more often than not it is easier to see if the uterus is anteflexed or retroflexed), and the presence of such complicating factors as fibroid tumors of the uterus. While a gestational sac is sometimes seen as early as during the 4th week of gestation, information technology may not be seen until the end of the 5th calendar week, when the serum HCG levels have risen to g-1500 mIU.
Gestational sac size may exist determined by measuring the largest diameter, or the mean of three diameters. These differences rarely effect gestational age dating by more a twenty-four hours or two.
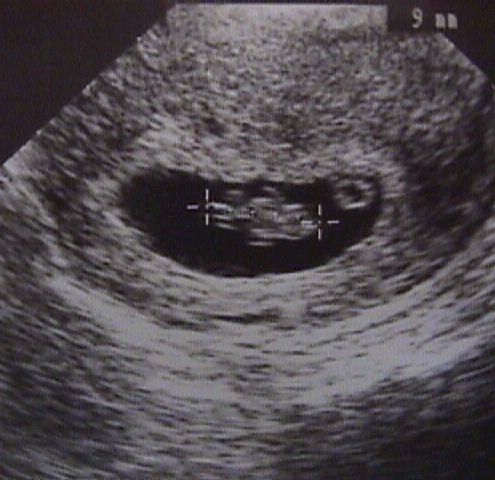
1st Trimester Ultrasound Scan
Yolk Sac
As the pregnancy advances, the next construction to go visible to ultrasound is the yolk sac. This is a round, sonolucent structure with a bright rim.
The yolk sac kickoff appears during the fifth calendar week of pregnancy and grows to be no larger than half dozen mm. Yolk sacs larger than 6 mm are commonly indicative of an aberrant pregnancy. Failure to identify (with transvaginal ultrasound) a yolk sac when the gestational sac has grown to 12 mm is also usually indicative of a failed pregnancy.
Yolk sacs that are moving inside the gestational sac ("floating"), comprise echogenic material (rather than sonolucent), or are gross misshapen are ominous findings for the pregnancy.
Fetal Heart Beat
Using endovaginal scanning, fetal cardiac activity is often seen fifty-fifty before a fetal cell mass tin be identified. The fetal cardiac muscle begins its' rhythmic contractions, and that rhythmic motility can be seen along the edge of the yolk sac. Initially, the fetal cardiac move has a slower rate (sixty-ninety BPM), but cardiac rate increases every bit the fetus develops farther. Thus, for these early pregnancies, the actual cardiac rate is less important that its presence or absenteeism.
Sometimes, with normal pregnancies, the fetal heartbeat is not visible until a fetal pole of upward to iv mm in length is seen. Failure to identify fetal cardiac activity in a fetus whose overall length is greater than iv mm is an ominous sign.
It can sometimes be difficult identifying a fetal heartbeat from the background movement and maternal pulsations. Y'all may find it useful in these cases to scan with i mitt while taking the maternal pulse with the other. This makes it easier to place sonographic movements that are dyssynchronous with the maternal pulse.
Fetal Pole
A mass of fetal cells, dissever from the yolk sac, starting time becomes apparent on transvaginal ultrasound only after the sixth week of gestation. This mass of cells is known as the fetal pole. It is the fetus in its somite phase. Ordinarily yous can identify rhythmic fetal cardiac motion within the fetal pole, although it may need to grow several mm before this is credible.
The fetal pole grows at a charge per unit of about one mm a day, starting at the 6th week of gestational age. Thus, a uncomplicated way to "engagement" an early pregnancy is to add the length of the fetus (in mm) to 6 weeks. Using this method, a fetal pole measuring 5 mm would have a gestational age of half-dozen weeks and five days.
Crown Rump Length
This term is borrowed from the early on 20th century embryologists who found that preserved specimens of early miscarriages assumed a "sitting in the chair" posture in both formalin and booze. This posture made the measurement of head-to-toe length incommunicable. Instead, they subsituted the head-to-butt length (crown rump length) as a reproducible method of measuring the fetus.
Early ultrasonographers used this term (CRL) because early on fetuses also adopted the sitting in the chair posture in early on pregnancy. Today, the crown rump length is a universally recognized term, very useful for measuring early pregnancies. The CRL is highly reproducible and is the unmarried most accurate measure of gestational age. Later 12 weeks, the accurateness of CRL in predicting gestational historic period diminishes and is replaced by measurement of the fetal biparietal bore.
In at least some respects, the term "crown rump length" is misleading:
-
For much of the first trimester, there is no fetal crown and no fetal rump to measure.
-
Until 53 days from the LMP, the most caudad portion of the fetal jail cell mass is the caudal neurospone, followed by the tail. Simply afterwards 53 days is the fetal rump the nigh caudal portion of the fetus.
-
Until 60 days from the LMP, the most cephalad portion of the fetal jail cell mass is initially the rostral neurospore, and afterwards the cervical flexure. Later on threescore days, the fetal head becomes the most cephalad portion of the fetal cell mass.
-
What is really measured during this early development of the fetus is the longest fetal diameter.
From half-dozen weeks to 9 1/2 weeks gestational age, the fetal CRL grows at a rate of about 1 mm per day.
| Gestational Age (Weeks) | Sac Size | CRL |
| 4 | three | |
| five | 6 | |
| half-dozen | 14 | |
| 7 | 27 | 8 |
| 8 | 29 | 15 |
| 9 | 33 | 21 |
| ten | 31 | |
| 11 | 41 | |
| 12 | 51 | |
| xiii | 71 |
Determination of Gestational Age
Measurement of the gestational sac bore or the length of the fetal pole (CRL) can exist used to decide gestational age. Charts have been developed for this purpose, merely some uncomplicated rules of thumb can also be effectively used.
-
Gestational Sac: Gestational age = iv weeks plus (mean sac diameter in mm x days). This relies on the growth of the normal gestational sac of 1 mm per day subsequently the 4th week of gestation. For example, a gestational sac measuring 11 mm would be approximately five weeks and four days gestational age. (iv weeks plus 11 days = 5 weeks and 4 days).
-
Crown Rump Length: Gestational age = 6 weeks plus (CRL 10 days). This relies on the growth of the normal fetus of 1 mm per solar day later on the 6th week of gestation. For instance, a CRL of 16 mm would correspond to a gestational historic period of 8 weeks and two days (half-dozen weeks plus xvi days = 8 weeks and ii days).
Twins
Twins
Twins and other multiple gestations can usually be identified adequately early on in pregnancy. They may be seen with two split gestational sacs (diamniotic, dichorionic twins). They may exist seen as two fetal poles occupying the aforementioned gestational sac (monochorionic twins). Information technology is useful to identify twins early as the prognosis varies, depending on the chorionicity and amnionicity of the twins.
A "vanishing twin" occurs in about 20% of twin pregnancies. In these cases, i of the twins fails to grow and thrive. Instead, its development arrests and information technology is reabsorbed, with no show at commitment of the twin pregnancy. It will prove useful to advise patients of this phenomenon who are establish to accept twins early on in pregnancy.
Missed Abortion
A missed abortion is an abnormal pregnancy that is destined to expel. Nigh one in v early pregnancies will non survive. These will grow for a while, with HCG in the urine and serum, simply eventually volition stop growing commonly, and and then will stop growing at all. Most of these (two-thirds) will accept aberrant chromosomes. Prove of a missed ballgame using loftier-resolution transvaginal scanning includes:
-
Absence of a visible fetal heartbeat when the CRL is greater than 5 mm.
-
Absence of a fetal pole when the average sac diameter is more than than eighteen mm.
-
Loss of fetal cardiac activity that was previously seen.
Read more almost missed abortion
Threatened Abortion
A threatened ballgame is whatsoever 1st trimester pregnancy that demonstrates uterine bleeding and/or cramping. Such patients are oftentimes evaluated with ultrasound. Bleeding in early pregnancy is a common event and is seen in 25 to forty% of pregnancies. Nearly one-half of these will keep to expel while the other half volition exist normal.
The benefits to ultrasound evaluation include:
-
Detection of abnormal pregnancies that are destined to expel.
-
Enabling scheduled intervention, if desired by the patient.
-
Enabling collection of pregnancy tissue for chromosomal analysis, if desired past the patient.
-
Reassurance to the patients with normal ultrasound scans.
Unfortunately, diagnosis of an aberrant pregnancy does not allow for intervention to right the abnormality.
In the presence of uterine bleeding, visualization of a gestational sac, a yolk sac, a fetal pole and fetal centre beat changes the risk of a threatened abortion leading to miscarriage from fifty/50 to about 5%.
Observation of subchorionic bleeding (claret outside the sac) is noted in about 20% of patients with threatened abortion. This is a worrisome sign, and reduces the pregnancy continuation rate to about two/3.
Read more nearly threatened ballgame
Incomplete Ballgame
Ultrasound is sometimes used after passage of pregnancy tissue to make up one's mind whether whatever pregnancy tissue remains inside the uterus. Findings will vary in these cases. Sometimes, information technology is obvious that at that place is zilch left inside the uterus, every bit evidenced past a thin, consummate endometrial stripe. In other cases, there will be obvious pregnancy tissue. In the remaining cases, some cloth will still be present within the uterus, simply it won't exist clear (on ultrasound) whether this is blood, claret clot, or retained products of conception.
Read more about incomplete abortion
Ectopic Pregnancy
Early on intrauterine pregnancies are relatively easy to see with high resolution transvaginal ultrasound scanning. Pregnancies outside the uterus (ectopic pregnancies) are more difficult. The appearance of the ectopic pregnancy itself is the same equally for intrauterine pregnancies. Depending of the gestational age and normalcy of evolution, you lot may come across a gestational sac, a yolk sac, a fetal pole, and a fetal heartbeat. The difficulty lies in finding the pregnancy without the normal uterine landmarks.
Using transvaginal scanning, nigh half of the ectopic pregnancies can exist directly visualized, but in the other one-half of cases, simply indirect evidence of an ectopic pregnancy will exist establish. Such indirect evidence includes:
-
Absence of an identifiable intrauterine pregnancy with maternal serum HCG levels of more than 1500 (this number varies and may be lower in some labs).
-
Presence of an intrauterine gestational "pseudosac." These sparse-walled structures represent some fluid (sometimes blood) within a decidualized endometrium that bears a superficial resemblence to a gestational sac. However, it lacks the bright echogenic ring of a true gestational sac and volition never incorporate a yolk sac.
-
Big amounts of free fluid (blood) inside the abdominal cavity. Pocket-size amounts of complimentary fluid are not-diagnostic, as this is commonly seen in cases of spontaneous abortion, ruptured ovarian cysts, and ovulation.
Read more than about ectopic pregnancy
Ovarian Follicle
Corpus Luteum Cyst
Following release of the egg, the ovarian follicle changes into a corpus luteum, responsible for product of hormones that will help support the developing pregnancy. The ascertainment of these small (usually less than 5 cm) ovarian cysts during early on pregnancy is essentially a normal finding. Should the cyst exist large (5 cm or more), or have suspicious characteristics, they may be followed every bit most corpus luteum cysts will resolve spontaneously sometime during the first trimester.
Non all ovarian cysts identified during the beginning trimester are corpus luteum cysts. Innocent paratubal cysts can be seen, requiring no treatment, equally well as ovarian dermoid tumors which can be more than threatening.
Nuchal Translucency Thickness
Late in the first trimester, an echolucent expanse tin be identified at the back of the cervix of normal fetuses. Normally sparse, it has been observed that an unusually thick translucency is sometimes associated with such abnormalities equally trisomy 21 and other fetal malformations.
Between the 11th and end of the 13th week of gestation, the measurement of nuchal translucency is obtained with the fetus in saggital section and a neutral position of the fetal caput (neither hyperflexed nor extended, either of which can influence the nuchal translucency thickness). The fetal paradigm is enlarged to fill 75% of the screen, and the maximum thickness is measured, from leading edge to leading edge. It is important to distinguish the nuchal lucency from the underlying amnionic membrane.
Normal thickness depends on the overall size of the fetus (CRL), but it should non exceed 3 mm at any gestational age. Among those fetuses whose nuchal translucency exceeds the normal values, there is a relatively loftier risk of significant aberration. Between 65 and 85% of trisomic fetuses will have a large nuchal thickness. Farther, other, not-trisomic abnormalities may also demonstrate an enlarged nuchal transparency. This leaves the measurement of nuchal transparency as a potentially useful 1st trimester screening tool, peculiarly in combination with biochemical screening. Abnormal findings allow for early careful evaluation of chromosomes and possible structural defects on a targeted ground.
This information is provided by The Brookside Associates. The Brookside Associates, LLC. is a individual organization, not affiliated with any governmental agency. The opinions presented here are those of the writer and do not necessarily represent the opinions of the Brookside Associates or the Department of Defense. The presence of any advertising on these pages does not constitute an endorsement of that product or service by either the United states of america Department of Defense or the Brookside Associates. All material presented here is unclassified.
C. 2009, 2014, All Rights Reserved
Source: https://brooksidepress.org/Products/Military_OBGYN/Ultrasound/1st_trimester_ultrasound_scannin.htm
Post a Comment for "Is It Good Tgat Gestational Sac Measuring Same as My Charting but No Baby 6.4"